Lymph node metastasis and lymphadenectomy of resectable adenocarcinoma of the esophagogastric junction
Introduction
Adenocarcinoma of the esophagogastric junction (AEG) is commonly regarded as a separated tumor entirety of upper digestive tract cancer (1). The incidence of AEG increases in both western and eastern countries (2). Surgery, based on Siewert types and with perigastric-mediastinal lymphadenectomy, remains a mainstream treatment for the resectable AEGs, and is of considerable interest (3,4). Siewert types are the well-accepted classification of AEGs, simply as the distal esophagus (type I), true carcinoma of the cardia (type II), and subcardial carcinoma (type III) (5).
Because biological behaviors of AEGs are different according to the tumor location, particularly the regulation of lymph node metastasis, the surgical procedures including the extent of lymphadenectomy are fairly controversial. The typical debate is whether AEGs should be treated via transthoracic or transhiatal approach (6). One of the major concerns is the dissection of lower mediastinal lymph nodes (7). Therefore, in this mini-review, we searched the database PubMed from January 2012 to May 2014 and summarized the novel and crucial findings of the behaviors of lymph node metastasis and optimal lymphadenectomy requirement for resectable AEGs.
Lymph node metastasis
Perigastric and mediastinal nodal metastasis
Perigastric regional nodal metastasis composes of the majority of all AEGs, such as no. 1 (25%), no. 2 (15%), no. 3 (25%), and no. 7 (13%) by an estimate, while lower mediastinal nodal (no. 110 and 111) involvement are 2%, respectively (3). The upper and middle mediastinal nodal involvement can be found but also rare (3). In certain estimates, among Siewert type I AEGs, 22.2-40.0% of patients have mediastinal metastasis, which commonly composed of half of the metastatic cases, but rare with upper mediastinal nodal metastasis (8,9). Kakeji et al. found higher incidence of upper and middle mediastinal nodal metastasis in Siewert type I AEG than those in type II and III, and the mediastinal nodal metastatic rate was obviously correlated with the length of esophagus invaded (10). The rates of peri-hiatal and mediastinal nodal metastasis from the identified literature were summarized in Table 1.
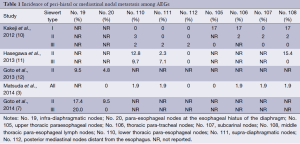
Full table
However, Siewert type II and III AEGs also respectively had 26.4% and 15.3% patients with mediastinal nodal metastasis (8). Likewise, Hosokawa et al. also reported relatively high rates of mediastinal nodal metastasis in type II and III as 21.3% and 12.5%, respectively (9). In contrast, in a Chinese series, the rates of mediastinal nodal metastasis were rare, only 4.7% and 0% in Siewert type II and III AEGs, respectively (13). Among both Siewert type II and III AEG patients, the incidences of metastasis are more than 10% at no. 1, 2, 3, 7, 9, 11p, and 19 groups, especially at no. 1 and 3 groups up to 37.0-52.5% (7). The nodal status appears similar between Siewert type II and III AEGs, which is the reason indicating normally identical surgical strategy for these two types.
Besides, with regard to the perigastric lymph nodes, undifferentiated AEGs more frequently metastasized than the differentiated did (10). For early-stage AEGs, the incidences of nodal metastasis in pT1a and pT1b diseases are 0% and 18%, respectively, and the positive nodes are all limited within lower mediastinum and perigastric D1 tier (14).
Siewert type II AEGs
Particularly, because Siewert type II AEG is located at a borderline area between thoracic and abdominal cavities, more attention is paid to its tumor biological behaviors. For Siewert type II AEGs, the nodal metastasis are 28-46% in first tier (along the lesser curvature, right cardia, left cardia and left gastric artery) and 13-18% in second tier (around the lower mediastinum, left renal vein, splenic artery and coeliac axis), respectively (15). A study included patients with advanced Siewert type II AEG undergoing radical esophagogastrectomy by thoracic-abdominal incision and two-field lymphadenectomy and investigated the status of nodal metastasis (16). The nodal metastasis rate was 75.6%, in which 57.0% only in abdominal field, 2.3% only in thoracic field, and 16.3% in both fields (14). The most frequent groups were no. 3 (46.5%), no. 1 (41.9%), no. 7 (17.4%), no. 110 (14.0%), no. 2 (10.5%), and no. 9 (5.8%) from high to low (16). Besides, thoracic nodal metastasis was associated with the vascular cancerous embolism among Siewert type II AEG cases (16).
Vena cava foramen (VCF) as a useful anatomic landmark
Besides, the exact location of the AEG sometimes is obscured in cases with large tumor size or hiatal hernia, but despite of the tumor size, the level where inferior vena cava passes through the diaphragm into the chest was introduced as a landmark to detect via computed tomography (6). Mine et al. studied relationships between the distance from the VCF to the proximal border of tumor and mediastinal lymph node involvement. The results indicated if the proximal border of tumor below VCF, lower mediastinal and abdominal nodal involvement were 23.1% and 76.9%, respectively, without upper or middle mediastinal nodal metastasis; while if above VCF, upper, middle, lower mediastinal, and abdominal nodal involvement were 22.7%, 18.2%, 18.2% and 72.7%, respectively (6). Therefore, the VCF can be considered as a useful anatomic level to predict the nodal status, especially for upper and middle mediastinal nodes.
Micrometastasis
Interestingly, Włodarczyk et al. studied the presence of micrometastasis in regional lymph nodes of patients with pN0 AEG, and found micrometastasis trended to be more frequent among Siewert type III AEGs (17). Critical methods of micrometastasis in this study were that nodes were harvested intra-operatively and examined using mixed monoclonal antibodies against pan-cytokeratins (AE1/AE3), while the definition of micrometastasis was single neoplastic cells or infiltration with diameter below 0.5 mm but not involving the interstitium (17).
Node staging
TNM staging system
AEG was previously staged as gastric cancer until the major revision in the seventh edition of the International Union Against Cancer (UICC) staging system, which classifies AEG as esophageal cancer (1). Currently, the common node staging is the standards according to UICC seventh edition, based on the number of metastatic nodes. However, the only difference of node staging between seventh edition of UICC TNM staging system in gastric cancer and esophageal cancer, is N3 disease further specified as N3a and N3b in gastric cancer (18). Based on the gastric cancer staging system, the prognosis is not able to be well distinguished between N2 and N3a subsets (1). In addition, for resectable N3 AEGs, they are only classified as stage IIIc diseases regardless of the tumor infiltration depth by the esophageal cancer staging system, but can be categorized into stage IIb (T1N3), IIIa (T2N3), IIIb (T3N3), and IIIc (T4N3) diseases by the gastric cancer staging system (18). Therefore, based on the esophageal cancer staging system, the prognosis of AEGs is better predicted between stage IIIb and IIIc subsets (1). Usually, pathological node (pN) stage can accurately predict the prognosis, but clinical node (cN) stage is weak to predict the survival outcome (19).
Metastatic lymph node ratio (MLR)
MLR is another useful staging approach to estimate the influence of node status on prognosis. Tang et al. found both N stage and MLR could be significant risk factors for early recurrence of Siewert type II-III AEGs after curable resection (20). Likewise, Zhang et al. found either pN or MLR stage could be used as an independent risk factor for 5-year survival outcome, while the hazard ratio of MLR stage trended to be greater than that of pN stage (21). However, the optimal cutoff(s) of MLR to classify distinguishing subgroups is still controversial and requires more evidence to confirm. Commonly used cutoff is 0.2, and patients with MLR higher than 0.2 have worse survival outcome (22).
Lymphadenectomy
Extent and approach of lymphadenectomy
In the latest version of Japanese gastric cancer treatment guidelines, for tumors invading the esophagus, D2 lymphadenectomy should include no. 19, 20, 110, and 111, namely the lower mediastinal lymphadenectomy (Figure 1) (23). In a Japanese series of operated Siewert type II-III AEG cases, extended total gastrectomy with transhiatal D2/D2+ lymphadenectomy composed of the majority (94.3%) (11). Moreover, lower mediastinal lymphadenectomy was performed through transhiatal approach in 81.3% of all cases, while the remnant was through transthoracic approach (11). Exactly, due to the low incidence of mediastinal nodal metastasis among Siewert type II-III AEG patients mentioned above, the transhiatal approach for mediastinal lymphadenectomy is more acceptable and safer. By the experience of Kakeji et al., despite of only 4.7% Siewert type I cases with mediastinal nodal metastasis, there was yet 23.3% patients undergoing transthoracic approach resection with more extensive mediastinal lymphadenectomy (10). However, in a German multicenter observation study, the mediastinal lymphadenectomy only composed of 47% among all AEGs, and in part it might reflect the current situation in general practice of surgical treatment (24,25).
Therapeutic value of lymphadenectomy
With the concept of therapeutic value for individual nodal dissection, the index is calculated by a format, index = metastatic rate of a certain nodal group × 5-year survival rate of corresponding metastatic cases. Some studies demonstrated that complete dissection of nodes at no. 1, 2, 3, and 7 groups of first tier had apparent greater therapeutic benefit than those at other groups for Siewert type II-III AEGs, estimated by therapeutic value indexes (3,7,11). In contrast, some of the second tier groups, including no. 8a, 9, 10, 11p, and 110, were also found beneficial to be dissected but the therapeutic value for survival was milder (3,7,11). Moreover, dissection of other mediastinal nodes except no. 110 seemed not beneficial in survival outcome.
Extended lymphadenectomy for Siewert type II-III AEGs
Hasegawa et al. performed a selected para-aortic lymphadenectomy of no. 16a2 lateral group, and found its metastatic rates of Siewert type II and III AEGs were as high as 5.4% and 22.2%, respectively (11). In particular, in the subset of Siewert type III AEGs, the 5-year survival rate was up to 25.0% among the no. 16a2 nodes dissected and positive cases (11). Mine et al. investigated the lymphadenectomy around the left renal vein among Siewert type II AEG patients, and found the incidence of left renal vein nodal metastasis is similar to that around the splenic artery, in the lower mediastinum and coeliac axis, with similar impact on patient survival (15). Interestingly, left renal vein lymphadenectomy was also found as an independent prognostic factor in patients with pT3-4 Siewert type II AEGs (15). Goto et al. stated splenectomy was mandatory in patients with Siewert type II AEG undergoing total gastrectomy in Japan, for the sake of thoroughly clearance of splenic hiatal nodes, and then found the metastatic rate of no. 10 group (at splenic hiatum) was 4.8% among the patients undergoing splenectomy (12). However, these procedures of more extended lymphadenectomy keep controversial and require larger studies to estimate.
Sentinel node (SN) navigation
Surgical SN navigation for AEG is a novel technique and might be useful in limited surgery for early stage AEG (26). A systematic review included 12 studies with a total of 492 patients, and found common methods of SN navigation were radionuclide, blue dye, computed tomography lymphography (26). The results demonstrated SN navigation was technically feasible with an acceptable detection rate and accuracy, and might be applicable in the cases of early-stage AEGs (26). Matsuda et al. used a dual tracer method employing radioactive colloid and blue dye to detect SNs among predicting early-stage Siewert I or II type AEG patients, and found SNs were successfully detected in all the patients, with the diagnostic sensitivity and accuracy on the SN status both 100%, and none SN were detected in lower mediastinum by intraoperative probing (27).
Survival outcome
Long-term survival after curative resection for AEG ranges between 18% and 50% (28). Lymph node metastasis or lymphovascular invasion are independent factors for poor prognosis of AEG patients after resection in curable intention (29). Sisic et al. found median survival time was not associated with number of nodes harvested, but significantly associated with pN stage or MLR stage among all Siewert type I-III AEGs (19). Among resected Siewert type II-III AEGs, the 5-year survival rates were 2.4% and 12.6% in high-MLR and low-MLR subsets, respectively, and also high-MLR was associated with worse median disease-free survival time and median survival time after recurrence (20). Siewert type II AEG had worse overall survival outcome than that of type I AEG, partially due to significantly more frequent nodal metastasis among type II patients (30).
Nakamura et al. found lower mediastinal nodal metastasis was an independent prognostic factor for poor survival outcome, and also was associated with distant metastasis in patients with Siewert type II-III AEGs (31). Hosokawa et al. also confirmed mediastinal nodal metastasis was a definite poor prognostic factor, and the independent risk factors associated with mediastinal nodal metastasis included esophageal invasion more than 2 cm and histological grade 3-4 (9). Stratified by AEGs’ proximal border below or above VCF, the 3-year recurrence-free survival rates of were 37.4% and 35.8%, respectively (6). Kakeji et al. found a shift of major recurrence pattern from mediastinal nodal metastasis in Siewert type I AEGs to peritoneal seeding in type III (10).
Additionally, a small size study found micrometastasis in the nodes from pN0 AEG cases was not associated with the survival outcome (17). Extranodal metastasis, i.e., carcinomatous node, in AEG patients is not few, as high as 24.6%, which is significantly associated with number of metastatic nodes and lymph node ratio (32). The extranodal metastasis is an independent and poor prognostic factor for AEG patients undergoing curable resection (32).
Summary
Based on Siewert classification, AEGs have different behaviors of perigastric-mediastinal nodal metastasis. Siewert type I AEGs have higher incidence of mediastinal nodal metastasis than those of type II or III, especially at middle-upper mediastinum. With regard to the necessity of mediastinal lymphadenectomy, theoretically, transthoracic esophagogastrectomy with complete mediastinal lymphadenectomy is suggested for Siewert type I AEGs, while transhiatal total gastrectomy with lower mediastinal and D2 perigastric lymphadenectomy is a standard surgery for type II-III AEGs. Nevertheless, the mediastinal nodal metastasis is an independent factor of poor prognosis for any type of AEG.
Acknowledgements
Funding: National Natural Science Foundation of China (No. 81372344 and 81301866); New Century Excellent Talents in University support program, Ministry of Education of China (2012SCU-NCET-11-0343). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Disclosure: The authors declare no conflict of interest.
References
- Kim HI, Cheong JH, Song KJ, et al. Staging of adenocarcinoma of the esophagogastric junction: comparison of AJCC 6th and 7th gastric and 7th esophageal staging systems. Ann Surg Oncol 2013;20:2713-20. [PubMed]
- Oda I, Abe S, Kusano C, et al. Correlation between endoscopic macroscopic type and invasion depth for early esophagogastric junction adenocarcinomas. Gastric Cancer 2011;14:22-7. [PubMed]
- Matsuda T, Takeuchi H, Tsuwano S, et al. Optimal surgical management for esophagogastric junction carcinoma. Gen Thorac Cardiovasc Surg 2014. [Epub ahead of print]. [PubMed]
- Gronnier C, Piessen G, Mariette C. Diagnosis and treatment of non-metastatic esophagogastric junction adenocarcinoma: what are the current options? J Visc Surg 2012;149:e23-33. [PubMed]
- Siewert JR, Stein HJ. Classification of adenocarcinoma of the oesophagogastric junction. Br J Surg 1998;85:1457-9. [PubMed]
- Mine S, Sano T, Hiki N, et al. Thoracic lymph node involvement in adenocarcinoma of the esophagogastric junction and lower esophageal squamous cell carcinoma relative to the location of the proximal end of the tumor. Ann Surg Oncol 2014;21:1596-601. [PubMed]
- Goto H, Tokunaga M, Miki Y, et al. The optimal extent of lymph node dissection for adenocarcinoma of the esophagogastric junction differs between Siewert type II and Siewert type III patients. Gastric Cancer 2014. [Epub ahead of print]. [PubMed]
- Xiao WG, Ma K, Peng L, et al. Characteristics of lymphatic metastasis and surgical approach of adenocarcinoma of the esophagogastric junction. Zhonghua Wei Chang Wai Ke Za Zhi 2012;15:897-900. [PubMed]
- Hosokawa Y, Kinoshita T, Konishi M, et al. Clinicopathological features and prognostic factors of adenocarcinoma of the esophagogastric junction according to Siewert classification: experiences at a single institution in Japan. Ann Surg Oncol 2012;19:677-83. [PubMed]
- Kakeji Y, Yamamoto M, Ito S, et al. Lymph node metastasis from cancer of the esophagogastric junction, and determination of the appropriate nodal dissection. Surg Today 2012;42:351-8. [PubMed]
- Hasegawa S, Yoshikawa T, Rino Y, et al. Priority of lymph node dissection for Siewert type II/III adenocarcinoma of the esophagogastric junction. Ann Surg Oncol 2013;20:4252-9. [PubMed]
- Goto H, Tokunaga M, Sugisawa N, et al. Value of splenectomy in patients with Siewert type II adenocarcinoma of the esophagogastric junction. Gastric Cancer 2013;16:590-5. [PubMed]
- Fu SJ, Fang WT, Mao T, et al. Comparison of outcomes after surgery between adenocarcinoma of the esophagogastric junction and lower thoracic esophageal squamous cell cancer. Zhonghua Wei Chang Wai Ke Za Zhi 2012;15:893-6. [PubMed]
- Gertler R, Stein HJ, Schuster T, et al. Prevalence and topography of lymph node metastases in early esophageal and gastric cancer. Ann Surg 2014;259:96-101. [PubMed]
- Mine S, Sano T, Hiki N, et al. Lymphadenectomy around the left renal vein in Siewert type II adenocarcinoma of the oesophagogastric junction. Br J Surg 2013;100:261-6. [PubMed]
- Li SM, Li ZY, Ji X. Clinical characteristics of lymph node metastasis in Siewert type II adenocarcinoma of the gastroesophageal junction. Zhonghua Zhong Liu Za Zhi 2013;35:288-91. [PubMed]
- Włodarczyk J, Mueller J, Włodarczyk J. Lymph node micrometastases of adenocarcinoma located in gastroesophagal junction. Pol J Pathol 2013;64:170-4. [PubMed]
- Edge SB, Byrd DR, Compton CC. eds. American Joint Committee on Cancer: AJCC cancer staging manual. New York: Springer, 2010.
- Sisic L, Blank S, Weichert W, et al. Prognostic impact of lymph node involvement and the extent of lymphadenectomy (LAD) in adenocarcinoma of the esophagogastric junction (AEG). Langenbecks Arch Surg 2013;398:973-81. [PubMed]
- Tang P, Zhang HD, Yu ZT. Risk factors of early recurrence and prognosis for patients with adenocarcinoma of gastroesophageal junction after curative resection. Zhonghua Yi Xue Za Zhi 2013;93:3594-7. [PubMed]
- Zhang HD, Ma Z, Tang P, et al. Prognostic value of metastatic lymph node ratio in adenocarcinoma of the gastroesophageal junction. Zhonghua Wei Chang Wai Ke Za Zhi 2013;16:822-6. [PubMed]
- Zhang YF, Shi J, Yu HP, et al. Factors predicting survival in patients with proximal gastric carcinoma involving the esophagus. World J Gastroenterol 2012;18:3602-9. [PubMed]
- Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2010 (ver. 3). Gastric Cancer 2011;14:113-23.. [PubMed]
- Steinert R, Gastinger I, Ridwelski K, et al. Surgical treatment of carcinomas of the oesophagogastric junction - results achieved in multicentre studies. Zentralbl Chir 2013;138:403-9. [PubMed]
- Chen XZ, Zhang WH, Hu JK. Lymph node metastasis and lymphadenectomy of resectable adenocarcinoma of the esophagogastric junction. Asvide 2014;1:244.
- Filip B, Scarpa M, Cavallin F, et al. Minimally invasive surgery for esophageal cancer: a review on sentinel node concept. Surg Endosc 2014;28:1238-49. [PubMed]
- Matsuda T, Takeuchi H, Tsuwano S, et al. Sentinel Node Mapping in Adenocarcinoma of the Esophagogastric Junction. World J Surg 2014. [Epub ahead of print]. [PubMed]
- Kofoed SC, Muhic A, Baeksgaard L, et al. Survival after adjuvant chemoradiotherapy or surgery alone in resectable adenocarcinoma at the gastro-esophageal junction. Scand J Surg 2012;101:26-31. [PubMed]
- Zhang H, Wang W, Cheng Y, et al. Adenocarcinomas of the esophagogastric junction: experiences at a single institution in China. World J Surg Oncol 2013;11:155. [PubMed]
- Reeh M, Mina S, Bockhorn M, et al. Staging and outcome depending on surgical treatment in adenocarcinomas of the oesophagogastric junction. Br J Surg 2012;99:1406-14. [PubMed]
- Nakamura M, Iwahashi M, Nakamori M, et al. Lower mediastinal lymph node metastasis is an independent survival factor of Siewert type II and III adenocarcinomas in the gastroesophageal junction. Am Surg 2012;78:567-73. [PubMed]
- Zhang HD, Tang P, Duan XF, et al. Extranodal metastasis is a powerful prognostic factor in patients with adenocarcinoma of the esophagogastric junction. J Surg Oncol 2013;108:542-9. [PubMed]



